When it comes to VBAC induction, you may get many opinions on whether or not it is safe. Although it’s ideal for labor to start on its own, VBAC moms can safely be induced and still have a VBAC.
According to ACOG, a prior low transverse C-section scar is not a contraindication to induction, other than the use of Misoprostol (Cytotec). Induction methods, including Foley balloon, Pitocin, and artificial rupture of membranes (AROM), may be used safely in most women.
The problem arises when a practitioner does not support induction on women with a prior C-section. If you go past your due date, or there’s a medical reason to start labor sooner, providers who don’t offer VBAC induction might suggest a repeat Cesarean.
In this blog, we want to talk about induction methods for TOLAC and which ones are best to improve your chances of having a successful VBAC. We’ll also talk about some ways to encourage labor to start naturally.
Originally published March 27, 2019, this article was updated and republished on February 1, 2021.
The Best Induction Methods for VBAC
As mentioned above, there are a few methods providers can use to induce labor for a VBAC. But, what is the best way, and when do providers decide it’s appropriate to intervene?
Here is a breakdown of the common VBAC induction methods
Pharmacological VBAC Induction Methods:
- Pitocin or oxytocin
- Mifepristone
Mechanical VBAC Induction Methods:
- Foley catheters
- Double-balloon catheters
- Artificial rupture of membranes (AROM)
Softer VBAC Induction Methods:
- Scraping or sweeping membranes
- Evening Primrose Oil to Induce Labor
- Nipple Stimulation
- Physical Activity or Sex
Due dates are calculated based on your last menstrual period and/or measuring the fetus via ultrasound. Your baby is considered “term” at 37 weeks and “post-term” between 41 and 42 0/7 weeks of pregnancy.
A study released in 2018 suggests that induction in week 39 is optimal, but The Arrive Trial didn’t study VBAC induction.
ACOG concludes that “Induction of labor between 41 0/7 and 42 0/7 weeks can be considered” and “Induction of labor after 42 0/7 weeks and by 42 6/7 weeks of gestation is recommended, given evidence of an increase in perinatal morbidity and mortality.”
Contemporary OBGYN
There are sometimes medical reasons that bring induction to the table before these gestational weeks. If your provider finds there is a medical reason for induction, don’t worry. Most of the time, all the induction methods listed below can be discussed and considered with your provider.
Foley Catheter Induction or Cook Catheter
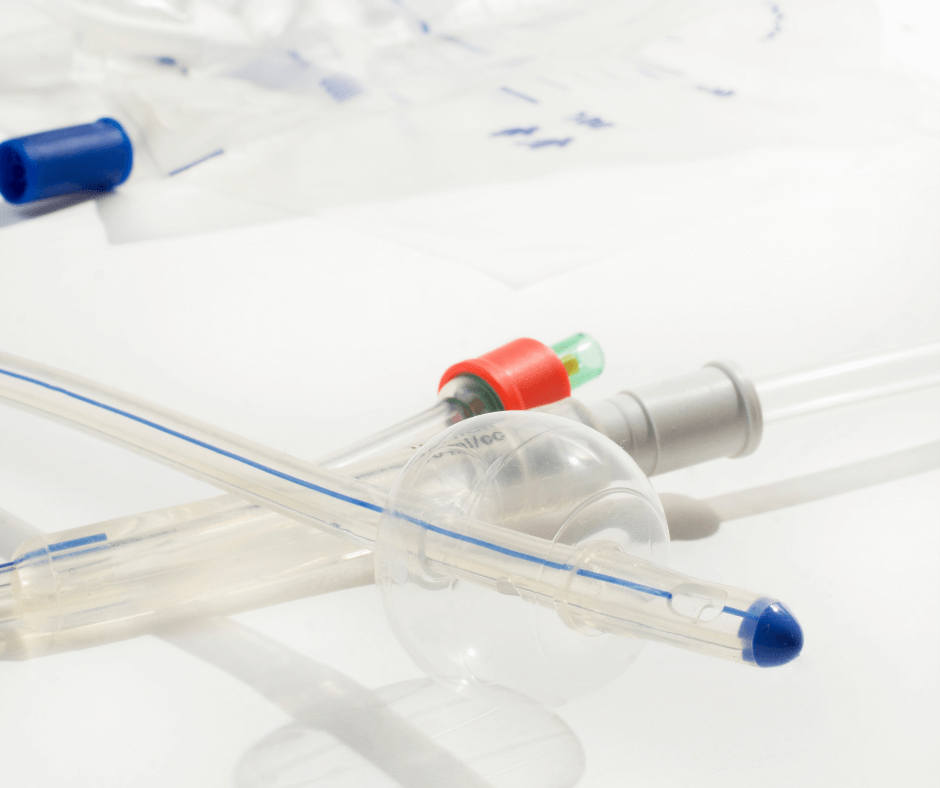
A gentle and effective way to induce VBAC may be a foley catheter induction. A foley or cook catheter is a small catheter that goes into the cervix.
There is a difference between a foley and a cook catheter. Attached on the end of a foley is a single balloon. Foley catheters are also used for other procedures such as urine output. A cook catheter has two balloons on the end of it.
No matter if it’s a foley or a cook catheter, they are both filled with saline solution after placement. The idea behind the foley/cook is to mechanically ripen or dilate by creating pressure on the cervix.
According to the Journal of Obstetrics and Gynecology research, a cook catheter shows significantly higher bishop scores on the success of the cervix ripening, vs foley bulb induction success.
A study shows that the rate of successful pre-induction resulting in delivery was 69.4%, with vaginal births accounting for 66.67% of all cases. Also, 30.66% of the pregnant women did not require the use of oxytocin.
Typically, the catheter is placed inside the cervix for up to 12 hours to allow the pressure to ripen the cervix.
One of the reasons why people choose to have a foley/cook induction is because it is a method that doesn’t require any medication, which some may consider important for a natural birth. It’s also more gentle on the mother and baby than some other induction methods may be.
It is not impossible, but much harder to place a foley/cook catheter into the cervix if it has not dilated or softened at all. A typical rule of thumb is that the cervix must be at least 1 cm dilated or soft enough to stretch for the catheter to enter.
A catheter induction may be uncomfortable while it is being placed because it is something going into a small space. Once it is placed, it can start contractions or cramps. These are good signs that it is working and helping the cervix become ready for your VBAC.
There have been providers who are unsure if a foley/cook catheter is a safe option for a VBAC induction. Studies have shown that a foley catheter or cook catheter is considered a safe and reasonable option for VBAC parents. I personally had a foley induction for my VBA2C, and I was grateful for that option. You can hear the story on episode 50 of our VBAC podcast.
Pitocin
Pitocin is a way that providers may choose to induce your VBAC. Pitocin is a synthetic version of Oxytocin, a hormone your body naturally produces.
Pitocin is administered via IV. Starting it low 1-2 ml an hour and increasing it slowly is considered a low dose. Pitocin may be a great way to gently encourage labor to start on its own.
Some providers are very uncomfortable with Pitocin as a VBAC induction method. Pitocin is not considered a contraindication for VBAC, but it is very important to not over-stress the uterus.
If it seems Pitocin is not working, providers may suggest moving on to C-section. However, there is an intervention called intrauterine pressure catheter (IUPC), that providers can use to measure your contractions.
When deciding whether it’s safe to continue trying for a VBAC, having accurate data can really help. Although not routinely used, IUPC is considered the most accurate way to measure uterine activity. It’s placed in the uterus and measures pressure within the amniotic space. Your water does need to be broken in order for a provider to place an IUPC.
It is a good idea to discuss with your provider their thoughts and availability to induce with Pitocin for VBAC. While Pitocin is generally considered safe for VBAC, some hospital policies may not allow a VBAC to be induced with Pitocin. Also, discuss how they will decide whether induction is working, so you’ll be prepared to make informed decisions.
Artificial rupture of membranes (AROM)
Some people are not offered many options when it comes to inducing their VBAC. Some providers may not offer any type of medical induction, however, they will suggest trying to break the bag of waters to encourage labor to start naturally.
When the bag of waters is ruptured, a small plastic “hook” is placed inside the cervix against the membrane. The provider then snags the membrane and punctures a small hole in the bag.
Once the membrane is punctured, it is common that amniotic fluid will leak out and release a hormone called prostaglandins. Prostaglandins mixed with oxytocin can help the body begin laboring contractions.
It is possible that labor will begin right away upon membrane rupture. However, there is a chance that it may take a while (up to 48 hours even). It’s also possible that it will not start labor at all because the body is not yet ready.
Breaking water is sometimes used if there are no other options provided. However, it may not be the most ideal intervention to start with, because the body may not be ready to begin labor at that very moment.
Gentle Ways to Induce Labor for VBAC

In addition to the medical ways to induce labor, there are other methods that may be considered to be more of a natural approach. These methods may or may not be successful.
NOTE: Be sure to consult with your medical provider to determine the best method for you.
Scraping or sweeping membranes
Stripping or sweeping of membranes is an option that can be done in an effort to get labor going without introducing any medication into the body. It is typically performed in the office of your care provider.
Your medical provider will insert their finger into your cervix and separate (sweep/strip) the amniotic sac from your uterine wall. This can release prostaglandins and stimulate labor contractions.
If it is successful, labor will typically start within 24-48 hours. It is possible that a sweep may not work at all or may take a few times before labor begins.
If the cervix is not as “primed” it may be an indicator that sweeping the membrane will be less successful. We encourage you to discuss the likelihood of it working with your provider to determine if this is a good step for you.
Evening Primrose Oil to Induce Labor
Evening primrose oil is extracted from the seed of the evening primrose plant. When due dates are coming up and induction looks like it may be necessary, many moms and midwives will suggest or look into Evening Primrose Oil (EPO).
The idea is to use it vaginally or orally to soften and ripen the cervix, preparing it for labor. In 2017, Evidence Based Birth ® posted a study showing that the people in the Evening primrose oil group had a longer first stage of labor. In 2020, Evidence Based Birth® released a podcast with updates on EPO usage that referenced a study showing that those taking EPO had a more favorable cervix at the onset of labor but had no effect on the length of labor.
It is important to note that both of these studies had less than 100 participates and neither of them studied the effects of EPO on VBAC, specifically. More research is needed to draw a definite conclusion.
Nipple Stimulation
Nipple stimulation produces that natural hormone we mentioned above, called oxytocin. While using a breast pump or manual stimulation, it is possible for the uterus to become stimulated and start labor.
Although it may start uterine contractions, they may not continue, and other interventions may be needed. That said, pumping to induce labor can be successful for some mothers.
Physical Activity or Sex
Going for a nice long walk or taking a shopping spree may be something that kick starts labor. Some providers will also suggest having sex. Physical activity and sex can increase your oxytocin levels and bring on contractions. Some may say it is a good idea to combine the two.
You can also try gentle movements, like pelvic tilts or bouncing on an exercise ball to induce labor.
It is important to remember if you choose this form of trying to induce your VBAC labor to not over do it. You do not want to go into labor feeling super tired. And always confirm with your medical provider before introducing a new activity.
Which Induction Method is Not Safe for VBAC?
Cytotec, also called Misoprostol is not considered a safe method for VBAC induction, due to an increased risk of uterine rupture.
In a case-control study of 512 women attempting VBAC, 5.6% of women receiving Misoprostol had symptomatic uterine rupture compared. Only 0.2% of those that did not use Misoprostol had a uterine rupture. Until more recent studies are conducted, Cytotec will continue to be a contraindication for VBAC induction.
DO NOT USE Misoprostol for VBAC induction.
Another cervical ripener known as Cervadil (Dinoprostone or PGE2) is a little more controversial on whether it is safe or not. One older study showed no increased risk of rupture for those using Cervadil as a cervical ripener, but the study only had 78 participants and is hardly conclusive.
If your provider suggests using Cervadil to ripen your cervix, it is a good idea to ask about the risks and benefits and the possibility of using other options such as the Foley Bulb, Cooks Catheter, or other methods as discussed above.
Why Do Some Doctors Not Support Induction After C-Section?

Despite the evidence and the ACOG clinical guidelines, the reality is that many doctors will still not agree to induction after C-section. WHY?
There may be many reasons, such as the one discussed in episode 6 of The VBAC Link Podcast. This mom shared that her doctor’s colleagues didn’t support him in taking her as a patient.
Doctors receive pressure from other co-workers and hospital administration. There are also hospital policies that they have to abide by, so it’s easier not to take a “risk” and avoid a potential lawsuit.
Even the doctor that told me we could induce in a gentle way said, “I’d need you to sign a form.” He said, verbatim, “You need to understand, I have a family too.” He felt that allowing me an induction after C-section was risky enough to put his own family at risk.
Although being induced does slightly raise risks for women who are having a TOLAC, it’s important to know your provider’s stance on it. Additionally, it’s important to know the methods they will use if they do medically need to induce.
Medical Reasons for Induction
Sometimes, there are true medical reasons why a mother would need to be induced. The 40-week due date or having a BIG baby are not necessarily reasons to induce. Read more about what ACOG has to say here.
There are also medical reasons that a TOLAC or induction is not the best method for delivery. If your provider suggests a scheduled C-section, or that induction is not a good idea, never hesitate to discuss the reasons and the evidence behind those reasons.
Here are a few of the medical reasons why your labor may need to be induced:
- Maternal medical conditions: Some medical conditions mean it’s medically no longer safe to be pregnant or no longer safe for a baby to be inside. Examples of these conditions may include gestational diabetes, RH-Blood disease, and chronic hypertension.
- Chorioamnionitis: Uterine infection.
- Preeclampsia/eclampsia: Pregnancy-related high blood pressure.
- Placenta Concerns: If the baby’s growth is extremely low, there are signs that the baby is in distress, the heart rate is not showing a safe pattern or abruption.
- PROM: Premature rupture of membranes when the water breaks and labor doesn’t start after 48+ hours.
- Fetal Demise: The passing away of the fetus.
Induction or C-Section?
The decision to have an induction for your VBAC or schedule a C-section can be a difficult one to make. We encourage you to learn more about what an elective C-section looks like, compare it with VBAC, and decide what is best for you and your family.
Our goal here at The VBAC Link is to help you build confidence and help you find all the facts surrounding both VBAC and C-section.
Induction can be a long and very emotional road, which may not be desired. We understand that completely. A family-centered Cesarean may be a preferable option.
We also want you to know that it is possible to be induced and still have a VBAC, like Patrice in episode 97 of our podcast.
Find a VBAC Supportive Provider (Who Supports TOLAC Induction)
When it comes to VBAC we truly believe that it is most important to have a supportive provider. This may be hard to find depending on your area or location.
Looking for a truly supportive provider, start by asking them their views on induction and TOLAC/VBAC. Ask what inducing a VBAC looks like to them, which induction method they prefer, and how they feel about it.
Although it’s better to go into labor spontaneously, and many women do so after the 40-week mark, it’s best to know your provider’s view in the beginning so you are prepared to handle circumstances that may come up.
Whether you decide to induce your VBAC birth or not, we are here for you. If you haven’t already, check out The VBAC Link Facebook Community, where people just like you are learning, growing, and deciding what is best for them.
Also check out the podcast episode all about Kimberly, who rocked an induced VBAC.
Learn more about how you can enhance your chances of rocking your VBAC with our Ultimate prep for parents VBAC course.
This course is a 100% online, video-based course that offers the world’s most comprehensive VBAC training in the world.













 Home Birth After C-Section: Deciding Between HBAC and Hospital Birth
Home Birth After C-Section: Deciding Between HBAC and Hospital Birth
Looking for more specific information information regarding Low dose pitocin. Is it 0.5 mU/min or 0.5 U/hr drip or some other rate. The Facebook group has lots of conflicting responses bc many don’t have units or the actual rate. Thank you!
Could you provide additional info on EPO risks? The abstract linked here doesn’t mention anything about uterine rupture or hemorrhage risk.
Trying for a VBA2C and I tend to go late in pregnancy so I’m wondering if laminaria would be a good induction along similar lines as the foley bulb? I vaginally delivered my stillborn daughter at 24/25 weeks between the Cs and they tried the laminaria for dilation but didn’t work because my body just wasn’t ready.
We do not have any solid information about laminaria for induction. I would recommend checking with your provider to make sure it is safe.
Do you have any studies on vbacs after multiple c sections? I am trying for my vba4c at the end of this month. All but my last incision were double layer closed my last one 2.5 years ago was only single. My care providers are concerned of a rupture but still willing to allow me to try for a vbac and they plan on doing sweeps twice a week starting at 37 weeks.
Hi! Yes, check out this article. https://www.thevbaclink.com/vbamc/
Hi, I have not been successful on finding much about Bandl ring. I had csection first time because of the ring. Is it possible for me to have Vbac during second pregnancy? Any success stories?