
As a doula, I’ve attended many births where scar tissue on the cervix causes labor to stall.
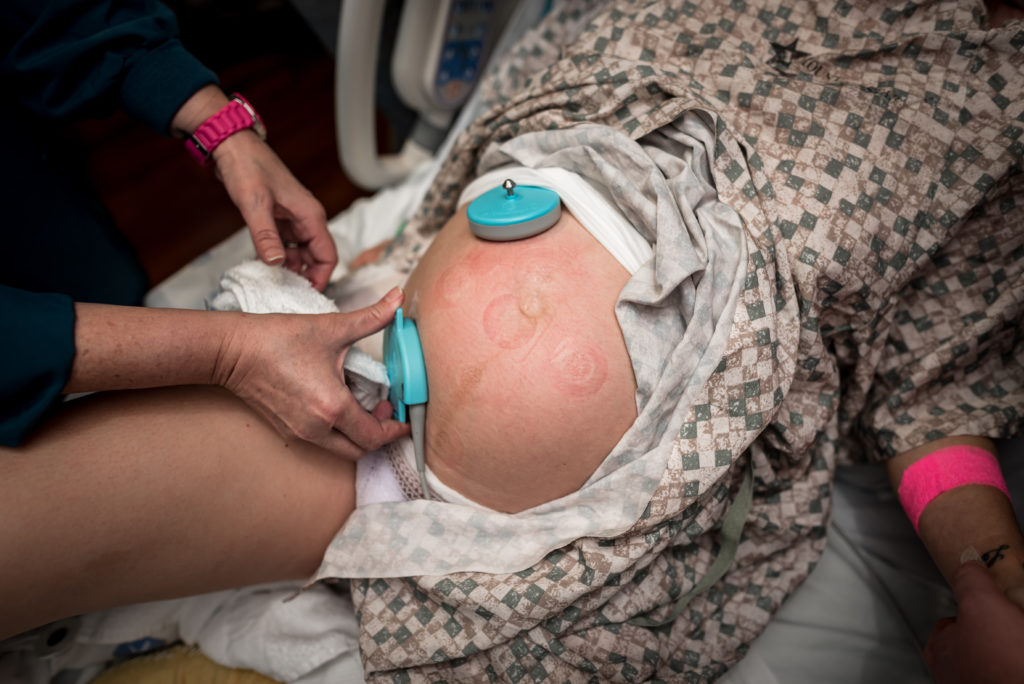
Here’s what it looks like.
Things are really intense for the birthing parent, maybe they even start making pushing or grunting noises, and I suspect transition may be happening. The nurse or provider will do a cervical check to see if it is time to start pushing. To much dismay, the mom is only 2-4 centimeters dilated.
Everyone in the room looks defeated, and sometimes, a decision to start an intervention such as Pitocin or an epidural is made.
Typically, as long as the baby is handling labor well, dilation starts happening again, progresses very quickly, and a baby is born. If issues like a posterior baby or transverse lie are ruled out, what’s causing labor to stall so early in dilation, while the mother is laboring so intensely?
Scar tissue on the cervix and the abdominal area can cause interruptions of the physiologic birth process. Yet, no one is talking about it. Excessive scar tissue on the cervix, uterus, bladder, or other areas of the pelvic floor can slow dilation, and lead to unnecessary interventions — up to and including becoming a reason for a C-section.
I personally believe that one of the biggest influencers of unnecessary Cesareans that happen due to failure to progress is scar tissue on the cervix.
So, let’s talk about it!
In this blog, you will find common causes of cervical scar tissue, how it impacts fertility and labor, what you can do about it, and the next steps to take if you suspect there is scar tissue on your cervix.
Can you get scar tissue on cervix?

Cervical scar tissue is exactly what it sounds like; scar tissue that forms on the cervix. It’s sometimes called adhesions, dense adhesions, or intrauterine scar tissue.
A more severe, but rare form of cervical scar tissue happens in the uterus and is called asherman syndrome. Asherman syndrome happens when adhesions or scar tissue form inside the uterus itself. It can occur in small areas of the uterus or, in the worst cases, adhere the front and back of the uterine walls together. The scar tissue can be thick or thin and can be scattered throughout the uterus or sit together in one large group.
The presence of scar tissue can be a factor in making a decision between VBAC vs repeat c-section.
Why do I have scar tissue on my cervix?
Scar tissue on the cervix can result from any pregnancy, type of delivery, surgical procedures in the pelvic floor area, and even inflammation. Typically, the following procedures and events leave some cervical scarring:
- Miscarriage or termination or pregnancy where a D&C or D&E was required
- Previous Cesarean birth
- Previous use of an IUD
- Hormonal birth control of one year or more
- A follow up procedure to an abnormal pap-smear such as a LEEP, Cyroposcopy, or Colposcopy.
- Use of Plan B birth control, even one time
- Previous vaginal delivery that results in a cervical tear
- History of sexual abuse or trauma
When there is trauma to the organs, such as surgery, the surface of the organs can become “sticky” causing them to adhere together. Sometimes the scar tissue can create web-like attachments between organs as the tissue continues to grow and the body heals.
Dense adhesions, or thick scar tissue, can cause organs to pull each other in a way that is not natural and can cause pain in the pelvis.
Intrauterine adhesions can interfere with the uterine lining, which may result in difficulty becoming pregnant, increased risk of miscarriage, or secondary infertility.
Signs of scar tissue on cervix
Unfortunately, scar tissue on the cervix can’t be diagnosed before labor begins, because a good amount of effacement of the cervix is needed for it to become apparent. Some people with cervical scar tissue may not have any noticeable issues. However, most women will experience abnormalities with menstruation or fertility.
Menstrual abnormalities and scar tissue on the cervix
Many women with cervical scar tissue have menstrual abnormalities like infrequent, light, or even absent periods. Rarely, if the adhesions block or slow down menstrual flow, it can lead to pelvic pain or intense menstrual cramping.
Fertility issues related to cervical scar tissue
Some people might not be able to become pregnant due to scar tissue impeding the sperm from getting to the egg, or prevention of the endometrium lining becoming thick enough for the egg to implant. Scar tissue can also cause recurrent miscarriages as the fetus grows into the scarred lining.
Rarely, depending on where the placenta implants in relation to scarring, problems during pregnancy and delivery can occur, such as placenta previa, accrete, or abruption.
How cervical scar tissue affects labor

During labor, there are some symptoms to be aware of, particularly if you know there is a history of the above-mentioned causes of scarring. These are some good indications that there may be scar tissue to be worked through:
- Feeling an overwhelming need to push but having low dilation
- A stall in dilation
- Effacement is high but dilation is low
- Mother is showing signs of being in transition but has dilation numbers of 5 or less
- Mother is having intense surges and is in labor but has no dilation at all
- Prodromal labor that starts and stops
- Water breaking after prodromal labor
If you are noticing these signs, there are a few things that can be done when in labor to help it progress normally and resolve. Your provider can massage the cervix during an exam. While uncomfortable for the birthing parent, it is very effective at loosening up the scar tissue enough for labor to progress.
In most cases, with less severe scar tissue, maternal movement and time will help the scar tissue soften up as labor progresses.
Another option for softening the tissue is inserting a Foley Bulb in the cervix and inflating it very gently. However, all of the things listed above would need a provider in the room with you who knows how to identify scar tissue on the cervix and is familiar with resolving it.
One thing that is very common after the release of cervical adhesions is that labor can progress very quickly. I have seen this happen with many clients. When there has been very little progress in dilation, but obvious signs of transition and pushing, I’ve seen babies arrive very quickly once the tissue is released, either mechanically or with time and patience.
Does cervical scar tissue mean you need a C-section?
Many times a diagnosis of failure to progress is attributed to unnoticed or untreated cervical scarring. As long as mother and baby are tolerating labor well, there is no need to rush a thing. Patience and movement can be all that is needed.
Trust in your body’s labor pattern, tune into your intuition, move as you feel the need to. Most importantly, find a provider that supports you and is willing to give you time to start labor on your own and allow it to progress on its own.
It is possible to have a natural, family centered cesarean, if it comes to that. Sometimes a C-section is simply unavoidable.
What to do next if you know you have scar tissue
There is no way to know if you have scar tissue on the cervix until labor starts. However, if you suspect you might have it, ask yourself these questions:
- Do you have a history of any of the procedures mentioned above?
- Have you had a Cesarean birth or a fast and intense vaginal birth?
- Do you have a provider who is familiar with cervical scarring (beyond LEEP procedures) and knows how to help resolve it?
- Is your provider willing to be patient if scar tissue stalls things during labor?
Things that can help
If you are concerned that scar tissue is present, there are some things you can do, in consultation with your doctor, to soften the tissue before birth.
Consider having sex frequently at the end of your pregnancy. Semen is a prostaglandin that helps soften the cervix and doesn’t come with the risks of evening primrose oil, Cytotec, or Cervadil.
Tampons soaked in castor oil can also help soften adhesions before labor starts. Again, only do this after consulting your provider.
In extreme circumstances such as Asherman’s syndrome, surgical removal of the adhesions might be recommended. The hard thing with surgery is that the scar tissue has a high chance of recurring, so it is only recommended with severe cases.
Many providers prescribe NSAIDs such as ibuprofen, naproxen, or high-dose aspirin to decrease the chances of excessive scar tissue forming.
Seeing a pelvic floor therapist during pregnancy and after delivery can help you identify if there are issues with intrauterine or cervical scarring. A skilled therapist can help you resolve these issues before labor even begins.
Cesarean scar massage is also very beneficial and can help loosen any problematic scarring before it becomes an issue. Learn more about pelvic floor therapy on our podcast, episode # 123 Cesarean Scar Massage and Care with Lynn.
Now that you’ve learned some of the really common experiences that can result in cervical scarring, you can start to understand how many C-sections might have been avoided with more patience and understanding.
If you’re worried about scar tissue affecting your labor and delivery, particularly if you’ve had a C-section in the past, we’re here to help!
Planning a VBAC birth? “How to VBAC: The Ultimate Prep Course for Parents” will teach you everything you need to know to have a smooth, successful birthing experience.
Register today, and get ready to be strong, thriving, and knowledgeable when your new baby comes.















 Laboring at Home: How to Stay Confident (And Safe)
Laboring at Home: How to Stay Confident (And Safe)
Very interesting read! This sounds like exactly what I went through in my 36 hours of very hard and horrible labour which resulted in a c section. Could endometriosis / adenomyosis also be considered a factor which would result in this??
Thank you for this article! I am currently preparing for my VBAC and this is great. That’s one more thing I can control! To massage my incision daily to help prevent this from happening. This makes me happy. Thank you. 🙂
I had an induced labor due to GD and had scar tissue on my cervix due to a leep procedure. After I had my epidural and Dr broke my water. I was not dilating. The babies heart rate dropped and I developed a fever it was game over. I had my c-section(not considered an emergency.) Is there any chance for a vbac or would it be safer to just repeat c-section?
After LEEP treatment back in 2012 I have been unable to have certain procedures to help with my fertility and have to undergo general anaesthetic due to tight/ closed cervix. (HGC and Embryo Transfer)
Never has anyone mentioned this could be a cause of infertility- i have other issues such PCOS that have been attributed to this! The one pregnancy I did have ended up ectopic in scar tissue from The right removed ovary and fallopian tube!
Could this be preventing sperm from entering my uterus? It does feel like it just comes out after sex – also is there anything I can do to help ease/remove it to open my cervix up more?
Yes Kathy McGrath, you would have to have a large enough dilation and sometimes incision to correct cervical opening size. Otherwise it will continue causing all sorts of issues if you’re not already experiencing any others. If you find a physician to do so, please post what you told them as far as the issues and who you went to, to have it corrected.
I had 2 c-sections and 1 very quick delivery plus a colposcopy. I’m not having any more kids but I can’t fit a mirena coil because of the scar tissue – the pain trying to get out in was worse than childbirth. Now that I’m peri-menopausal, I’d like to have one fitted. Any advice of how to go about that?
The recommendations given are more for women already pregnant. If I’m getting ready for pregnancy, what advice do you have since I would not be limited in what could be done to resolve any issues?
Hi Alex! Do you suspect that you have scar tissue on your cervix?
I’m curious who to go to and how to get the scar tissue broken up enough that you aren’t having severe constant contractions and pain and other sexual issues induced due to such. I was lied to and bullied into such procedure by my ex mother in law who was very jealous of me getting to homeschool my children, nursing or pumping for them so much that she was tripping my breast milk freezers and had bullied me into a LEEP prior to my 2nd conception with her son. Had I know she was lying to harm me, I would have gladly left. And never spoke to any of them again which I have now thankfully done so but having severe issues from it debilitating issues keeping me from working at all, and would like to get it corrected and remarry someone asking to. Can’t without it corrected and the issues resolved. The last 2 who said they’d do a dilation, perforated my uterine wall instead and did laparoscopy incisions twice now in 2 different spots both times after uterine perforation was done to me. I grew up in an extreme amount of abuse and don’t want anymore abuse and trauma in my life and praying to find someone who would respectfully correct it. I don’t know who to ask though a d have tried. They keep saying it isn’t the issue when it is. The last one has a very small amount passing but still not without straining and also told me that there is an umbilical bulge from straining so much for 12 years with nonstop contractions and blackouts and other issues that haven’t stopped and couldn’t get any air into my lungs as far as a deep breath causing me to pass out. Some of the issues have lessened but still blocked and causing many. Praying to start trying this year for more children before I’m too old to. Just turned 44. If you recommend anyone who would correct it, please let me know! I saw someone say they’ve had a doctor correct theirs but they didn’t give info as to who they went to. One claims to do so but said they travel and offer appts and were offering a hospital apartment surgery sounding rather sketchy. Praying to ASAP so I can start trying for more kids to homeschool in peace, as my marriage was far from that and would like a few more kids, hopefully a daughter especially, for the next 5 years of trying prayerfully.
It would have to be dilated and opening size corrected.
Such a helpful article! I had my third unplanned cesarean in September after 68 hrs of labor, having signs of transition and feeling pushy too soon multiple times throughout labor, never progressing past 9cm, and my cervix hardening during contractions towards the end of labor, so we suspect scarring/adhesions is why. Before this pregnancy I had done a lot of scar massage and cupping as felt in had adhesions. During this pregnancy I used evening primrose oil to in case I did have scarring on my cervix, still ended in a c-section. I’m planning on seeing pelvic floor PT, other than that is there anything else I can be doing before getting pregnant again?